How Organized Medical Records Make Doctor Visits More Effective: Research-Backed Communication Gains

Preparing for a doctor’s appointment often feels overwhelming. You scramble to gather scattered PDFs of lab reports, discharge summaries, and old prescriptions. During the 15-minute slot, you forget key details or struggle to explain your history clearly. The doctor spends precious time piecing together incomplete information instead of focusing on your concerns. This common frustration: pre-appointment stress; affects millions and can lead to missed details, repeated tests, or suboptimal care.
Organized personal health records (PHRs) or patient-accessible electronic health records (EHRs) change this dynamic. When patients bring a complete, searchable history to the visit, communication improves, decisions become more collaborative, and visits turn productive. Multiple peer-reviewed studies confirm these gains in patient-centered communication, relationship quality, and visit efficiency. Below, we explore the evidence and show how a tool like MedIQGPT puts this research into practice.
The Evidence: What Studies Show About PHRs, Communication, and Better Doctor Visits
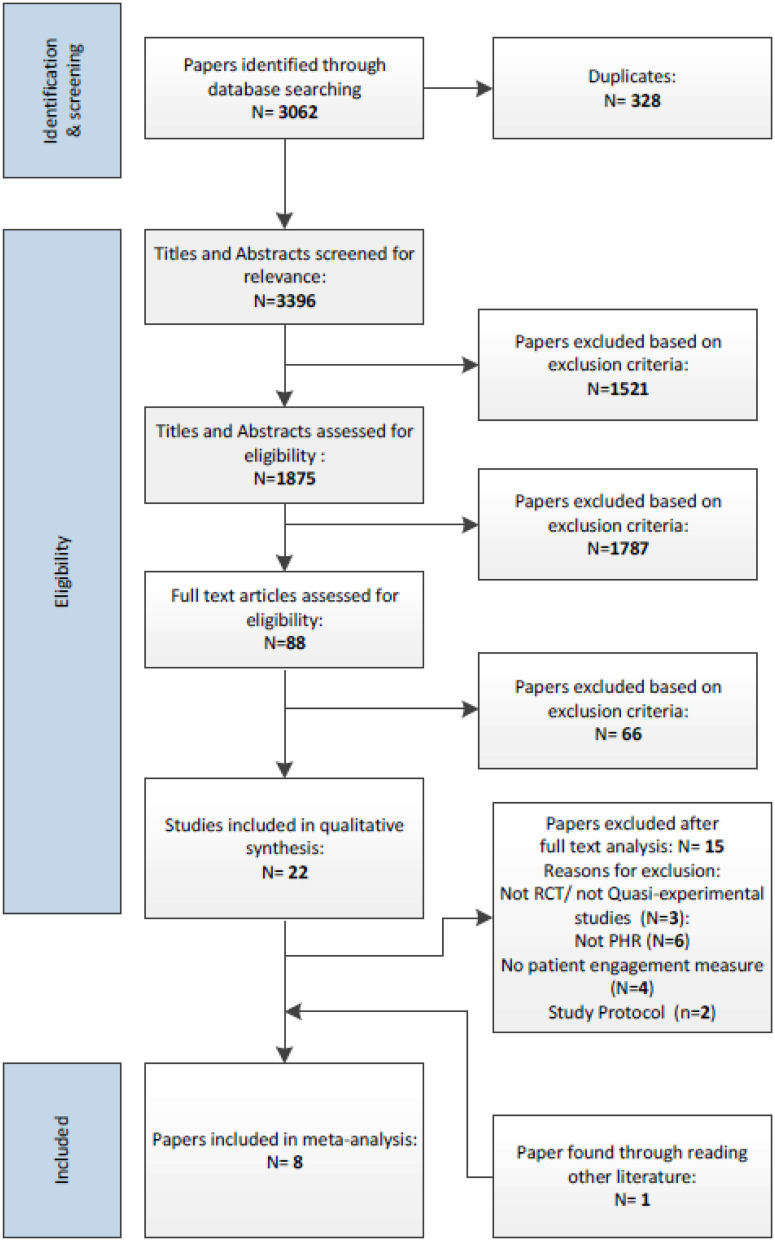
Systematic reviews and large-scale analyses consistently link patient access to their own medical records with stronger physician-patient interactions. A 2013 systematic review of 27 studies (including 20 randomized controlled trials) examined the effects of providing patients access to their medical records paper or electronic. Researchers found that accessible records improve patient-provider communication in several ways. For instance, pregnant women carrying their full antenatal records reported greater ease talking with doctors and midwives, feeling more involved and in control of their care. Other trials showed that sharing a specialist’s letter or computerized summary with patients boosted satisfaction with consultations and helped patients ask better questions.
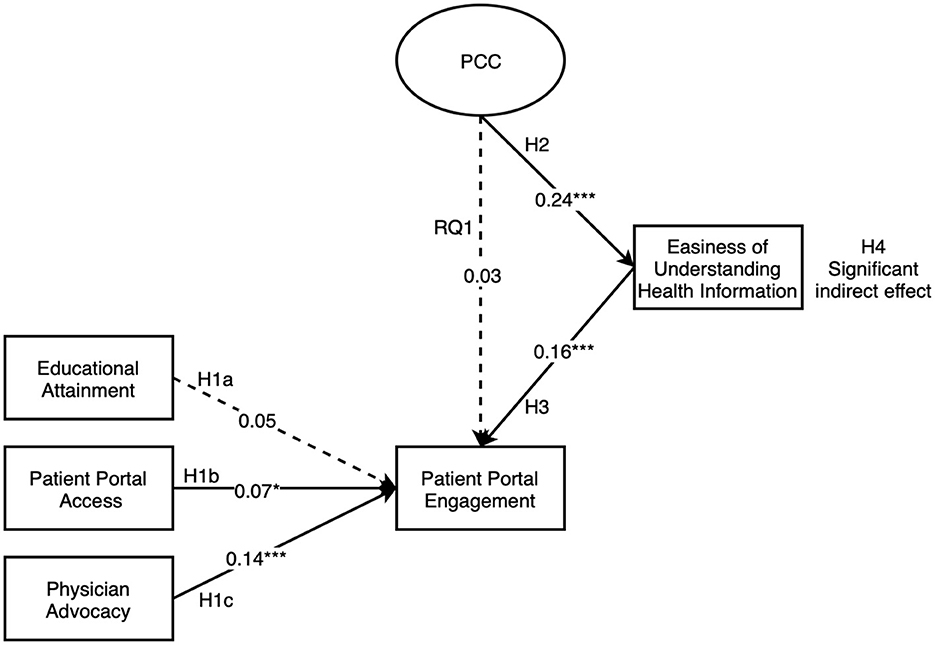
Patient-centered communication (PCC): the kind where doctors truly listen, explain clearly, and involve patients in decisions also benefits indirectly. A 2024 analysis of national Health Information National Trends Survey (HINTS) data from 1,251 adults used path analysis to test relationships. Patient-centered communication from doctors did not directly predict higher use of patient portals (a form of PHR). Instead, it had a significant indirect effect: better PCC made health information easier to understand (β = 0.24, p < 0.001), which in turn drove greater portal engagement (β = 0.16, p < 0.001). The indirect effect size was 0.04 (95% CI: 0.02–0.05). In practical terms, when doctors communicate well, patients feel more confident using their records leading to better-prepared visits and more meaningful follow-up discussions.
PHRs further strengthen relationships by giving providers quick access to shared history. A 2022 qualitative study involving colorectal cancer survivors, caregivers, and providers found that PHRs with secure messaging and journaling features help patients share symptoms, emotions, and treatment experiences asynchronously. Patients described this as reducing isolation and enabling collaborative decision-making. Providers appreciated having a fuller picture of the patient’s journey, which improved continuity across multiple specialists. Both sides noted that PHRs serve as “memory tools” for reviewing test schedules and side effects before appointments, prompting more focused questions and reducing recall errors during the visit itself.
A 2025 systematic review of PHRs and patient activation (a measure closely tied to engagement and self-management) reported an overall standardized mean difference of 0.41 in activation levels when patients used PHRs. While results varied by study design, the review highlighted that tools offering easy access and interpretation features help patients arrive at appointments more empowered and informed.
Finally, complete records reduce information gaps that lead to redundant tests or inefficient care. When patients can instantly reference trends in lab values or medication history, doctors spend less time reconstructing timelines and more time on diagnosis and planning. While one older study in the 2013 review found no direct drop in redundant testing, broader literature on care continuity shows that organized PHRs minimize duplication by ensuring everyone works from the same accurate history. Patients with chronic conditions especially benefit, as fragmented records often cause unnecessary repeats of blood work or imaging.
In short, the research is clear: when patients bring organized records, visits shift from reactive Q&A sessions to proactive, patient-centered conversations. Communication quality rises, relationships deepen, and care becomes more efficient.
How MedIQGPT Turns Research into Reality: The Doctor-Sharing Workflow
MedIQGPT is designed exactly for this evidence-based workflow: secure, simple, and built around real patient needs.
Here’s how it works in practice:
- Upload and Organize Once: Drag-and-drop PDFs, images, or DOCX files (lab reports, prescriptions, discharge summaries, imaging). The app automatically categorizes everything by type and date. No more hunting through email inboxes or dusty folders.
- Gain Instant Insights with ClinIQ: Before your appointment, ask the AI in plain English: “What was my hemoglobin trend last year?” or “Explain this lipid panel in simple terms.” ClinIQ interprets results, spots trends, and even suggests smart questions to ask your doctor directly supporting the preparation gains seen in studies.
- Share Securely with Doctors: Generate a view-only sharing link for your profile. Your doctor opens it on any device no account required and sees your complete, organized history instantly. You control access and can revoke it anytime. For specialists or insurance, use one-click batch export of selected records.
- Family and Multi-Profile Support: Manage up to six profiles (ideal for dependents) with granular controls. Share only what’s needed without exposing everything.
All data stays private with AES-256 encryption at rest and TLS in transit. Row-level security ensures only you (and explicitly shared parties) can access it. This privacy-first design addresses common concerns while enabling the communication benefits proven in research.
Patients using MedIQGPT report in our beta launch arrived better prepared. One doctor noted: “My patients who use MedIQGPT come better prepared to appointments. The shared profile feature gives me instant context without the usual back-and-forth.” This mirrors the relational and efficiency gains documented in the studies above.
Why This Matters for Your Next Appointment
Disorganized records waste time, erode trust, and can lead to gaps in care. Organized PHRs flip the script: they empower you, strengthen partnerships with your doctor, and support better health decisions. The evidence from systematic reviews to large national surveys shows measurable improvements in communication, engagement, and visit effectiveness.
Ready to experience the difference? Batch-export or share securely with MedIQGPT before your next appointment. Upload your records today, prepare with ClinIQ, and walk into your doctor’s office with confidence. Your health history deserves to work for you not against you.
Start free at Install MedIQGPT and upgrade to Pro for unlimited storage, doctor sharing, batch export, and full ClinIQ access.
Your next visit will thank you!
References